Managing Disc Herniation and Alleviating Sciatica: Tips and Tricks 1
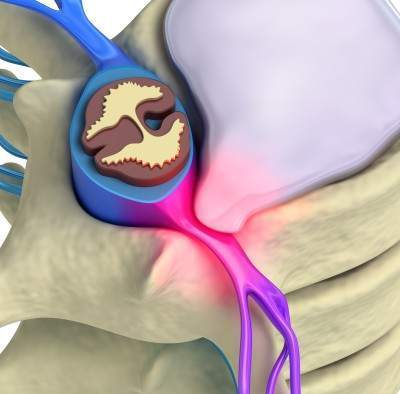
Suffering from disc herniation? Experiencing sharp pains shooting through your buttock, thigh, and leg due to sciatica? If your daily routine is disrupted by the discomfort of disc herniation, there’s hope. Many people find relief without needing surgery. This post will guide you through lifestyle changes to support your recovery from disc herniation. Stay tuned for our next piece, where we’ll explore exercises to correct and stabilize your condition.
Ultimate Guide To Exercises For Lumbar Disc Herniation Relief
Mary’s Story: A Wake-Up Call
Imagine starting your day like any other, performing your routine toe touches, when suddenly you’re hit with an excruciating pain radiating from your lower back down to your toes. This was Mary’s reality when she encountered a lumbar disc herniation, commonly referred to as a slipped or ruptured disc. Such incidents can lead to what’s known as sciatica or radiculopathy, terms doctors use to describe the pain that extends down your leg.
Understanding Lumbar Disc Herniation:
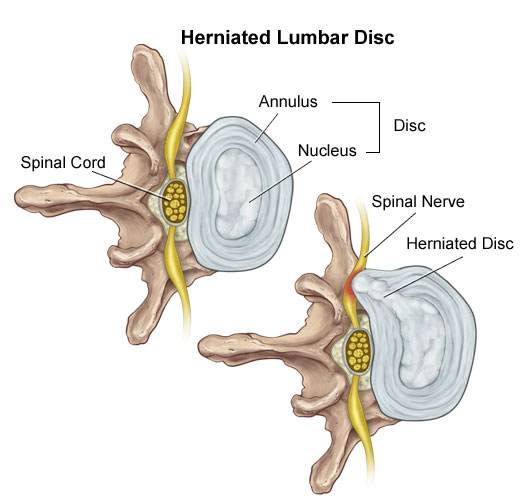
A glimpse into the anatomy of a herniated disc reveals two main components: the tough outer annulus and the softer, inner nucleus. Dr. Stuart McGill likens the nucleus to sticky phlegm. When Mary bent forward, it was akin to squeezing the front of a jelly doughnut, pushing the inner material backwards and eventually causing the disc to bulge and press on a nerve.
The Culprit Behind the Pain:
Mary’s disc herniation wasn’t a sudden mishap but the result of years of repetitive motions like toe touching and prolonged slouching at her desk. These habits gradually weakened her disc, leading to the moment when it finally herniated and impacted her nerve. The lack of nerves within the disc itself means significant damage can occur without immediate pain, explaining why the problem might not be felt until it’s severe.
A Lesson Learned:
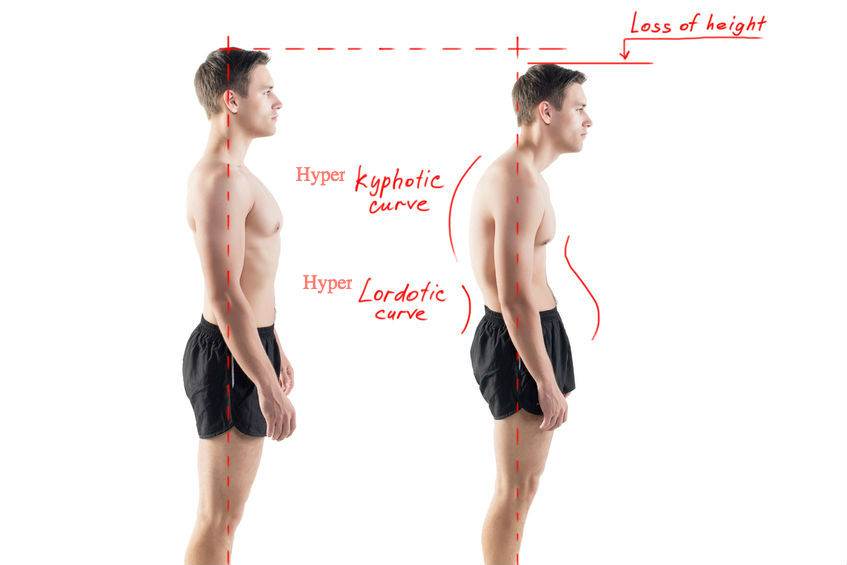
The story underscores the importance of posture and the dangers of neglecting spinal health. While the advice to “sit up straight” might seem simplistic, maintaining the natural curve of your back is crucial. Mary’s experience serves as a potent reminder of the long-term consequences of poor posture.
Disc herniations don’t have to dictate your life. By understanding the causes and adopting preventive measures, you can manage and alleviate your symptoms.
Understanding Disc Herniation: Pain, Prevention, and Care
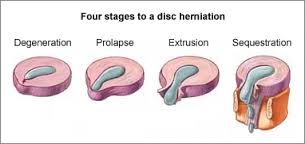
The Unseen Progression of Disc Herniation (see picture above)
- Bulging Disc: Early stages where the disc starts to protrude due to wear and tear.
- Prolapsed Disc: The disc bulges more as it degenerates, but the nucleus remains contained.
- Extruded Disc: The protective layers give way, pressing on nerves and causing pain.
- Sequestrated Disc: The most severe stage, where disc fragments break away, potentially compressing nerves or the spinal cord.
See Also: MRI, CT scan and X-rays: Is an MRI, CT Scan or X-ray Best For My Pain?
Why Me? The Role of Movement and Genetics in Disc Herniations
Surprisingly, your daily habits and genetic makeup play pivotal roles in disc health. While we can’t choose our genetics, modifying daily movements can significantly reduce the risk of herniation. Proper lifting techniques and posture adjustments are crucial first steps.
Simple Changes, Major Impacts: Daily Habits and Exercise
To protect your spine:

- Adjust Daily Habits: Learn to perform everyday activities in spine-friendly ways to prevent further disc damage.
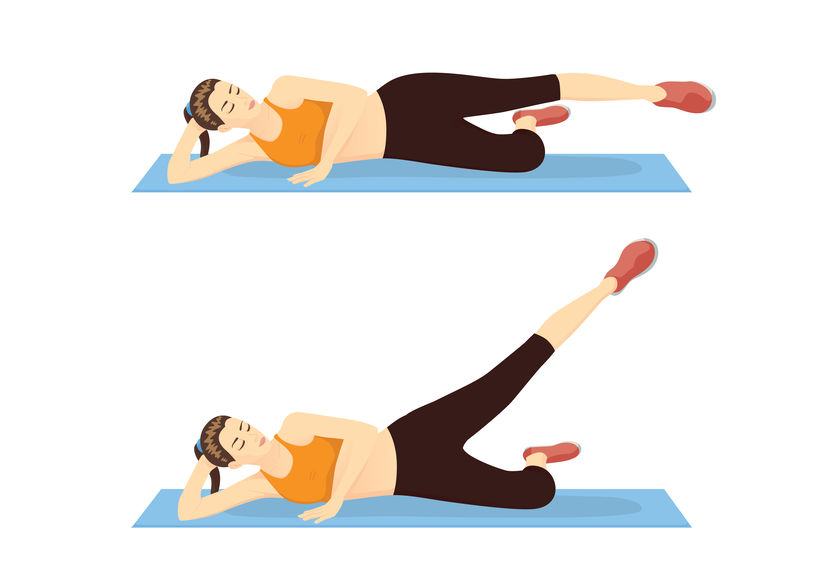
- Disc-Specific Exercises: Exercises can help reposition the herniated disc.
- Stabilization Routines: Strengthening your core helps maintain spinal integrity, preventing future herniations.
Lifting Techniques: How Weight Lifters Should Lift
Master the Basic Butt-Lifting Technique for Disc Health
- Practice with a long, straight object to ensure your back remains aligned.
- Ensure it touches your butt, mid-back, and the back of your head during the entire motion.
- Squat down and maintain contact with 3 areas and keep the lower back arched the whole time.
- Aim for 30 repetitions to embed this healthy habit into your daily routine for 10 days
Daily Activity Guide: Protecting Your Discs
Then you integrate this lifting technique into everyday life. Initially, whenever you do any of these activities, use the same basic move and you will stop pushing out your disc.
In the beginning, you will need to be conscious each time you are doing any of these activities. To speed things up you can practice each activity like picking up your socks 30 times using the butt lifting technique and it will become even more automatic. You can deepen muscle memory during all of these activities.
For sitting in a chair and driving I recommend that you roll up a Mckenzie Lumbar support roll and put that in the arch of your lower back
Guide for disc herniation daily activities.
- Remember to do all these movements pain-free. Always stop whenever you run into pain with any movement of the spine.
- Disc herniations are linked with long periods of sitting, especially prolonged driving.
- Disc herniations are caused by repeated flexion.
- Prolonged trunk flexion or twisted or bend sideways cause disc herniations.
- Too much lifting, pushing/pulling causes disc herniations
- Vibration while sitting is linked to disc herniations.
- After prolonged stooping or sitting, you should stand. For example, a gardener lifting bags of peat moss after having a prolonged period of rounded lower back, or a driver getting heavy loads out of the trunk after a long drive is not recommended. You should remember to stand for a few minutes before attempting to lift. Studies have shown that ½ hour is even better.
Here are some more exercises that can cause disc herniation.

Activities That Put Out Lumbar Disc Herniations
Yes, it’s very surprising that toe touches, Yoga and certain Pilates can cause disc pressure leading to disc herniations. I have personally treated dozens of Yoga teachers with varying degrees of experience. The fact is some of the exercises involved in Yoga are great for helping disc herniations while others directly push the disc out.
Many Yoga Exercises Put Out Disc Herniations
I know many Yogis who have had to stop many of their exercises due to the pain it cause them in various parts of the body, including their disc.
Next week’s article will go over the second and third ways to help your disc. Remember, you need to do #1 “Daily Disc Activities Correctly” first so that your disc doesn’t keep getting aggravated. Then you can move on to next week’s article which goes over #2 Disc Exercises to Push the Disc Back In and #3 Stabilization Exercises help by keeping the disc from coming out by normalizing how your spine moves.
Looking Ahead: Comprehensive Care for Disc Health
Next week, we delve deeper into specific exercises for disc realignment and stabilization techniques, in this article called Ultimate Guide To Exercises For Lumbar Disc Herniation Relief. Remember, starting with correct daily activities is essential to prevent aggravating your condition further.
Tell us what you think in the comments below and like us on Facebook. This Toronto Downtown Chiropractor will answer all questions in the comments section.




Hi! Thanks a lot for all this wonderful info! Really helpful! What would be the best way to put your shoes,trousers,socks on? Iam gathering some tips for my mom who was diagnosed with bad disk h. And advised to be operated 🙁
Author
Thanks for your question Adrianna. Simply sit down put an arch in your lower back, maintain the arch and put on your sock. For those that have excellent balance: Stand and maintain the curve in your lower back, lift one leg up and put on your sock or shoe.
Hope that helps your mother’s disc herniation.
Hi Dr. N.
I’m recently been given a pretty terrible back diagnosis: have just been diagnosed with grade 1 spondylolisthesis, almost complete degeneration of my L5 disc, and “severe” bilateral foraminal narrowing. Needless to say, I’m in some pain: for about 9 months now I’ve been trying to recover from a possible disc herniation, and while I’m on the upside of the curve at present, I’m still suffering from significant back pain, sciatica, numbness/tingling at times, yada yada. I’m off pain meds, but I’m yet to regain my full healthy lifestyle.
I’ve bought McGill’s new book Back Mechanic, and am finding it helpful. Have been doing his “Big 3”, as well as clamshells, single-leg lunges, and some hip flexor stretches. They were all immediately helpful, and have really helped me turn the corner. However, I feel that I’ve plateau-ed to some extent. I know the body tends to “get used to” certain action patterns, and I wonder if I need to move on to different exercises, or different progressions. Should I simply be doing more and more and more and more and more repetitions of these exercises (how much time is there in the day!?), or are there other exercises that can help me to get onto the next rehabilitation milestone?
Thanks,
Matt
Author
Thanks for your question Matt. The question in your case is the spondylolisthesis causing the pain or foraminal narrrowing. If you extend your spine 5-10 X like this exercise https://www.bodiempowerment.com/herniated-disc-part-2-the-best-exercises-for-your-herniated-disc/
Look for the McKenzie push ups. If you do those exercises 5-10X they way I describe and you are worse than the spondylolisthesis is likely causing your pain. If you get relief than relief than it’s a simple disc. If that is the case knee to chest exercises that you hold for 1 sec and you do repeatedly may help you. However like any exercises they have the potential to make you worse.
My take is that you need more stablization exercises and that the ones you are doing need to be more advanced. Likely that is the solution to your case. However without examination I cannot tell you for sure. Just go to the best chiropractor or physiotherapist in your area that you can find and they will set you up. Ask if they do rehabilitation and ask questions before hand so you don’t waste your money.
Hope that helps your disc herniation.
Dear Dr Ken Nakamura
I have a slipped disc at L5-S1 diagnosed with MRI and by a orthopedic 3 weeks ago. Previously I think I did have sciatica but it was not constantly there. I was seeing a chiropractor as I had a back pain which prevented me from bending forward to brush teeth back in 2015 (but have never really taken any MRI or Xray). My chiropractor told me there is no need to take the MRI/Xray and I have scoliosis hence part of my spine maybe stressed. I read online that 90% of people have some form of minor scoliosis. I do not have very obvious curvature hence I really didn’t understand if scoliosis is the cause of my slipped disc.
Moving forward, I didn’t realised that Downward Dog can cause Disc Herniation?! Because I continued practising this pose despite occasionally feeling the pull down my left leg. When I do downward dog, my back is slight arch (not flexed) as I am relatively flexible. Of course I am unable to practice yoga at the moment, as I really need to be patient and let my back heal.
My question is can I practice the lifting technique you taught on this page at this moment?
I am still on nerve repair supplement and medicine. My orthopedic taught me simple stretches such as knee to chest, easy twist and piriformis stretch and hamstring stretch. All these stretches to be done gently and to my best ability and in the specific order given. Perhaps I should practice this lifting with fewer than 30 repetition as my left knee is currently weaker (previously i injured my meniscus, and with my sciatica, I am standing a lot more as my sciatica gets trigger during certain sitting position. My knee is now feeling the strain.)
I will keep reading your site and get more information. Thank you.
Author
Thanks for your question Kit. If sitting aggravates your problem knee to chest exercises and hamstring exercises are not for you. An orthopedic surgeon is a specialist in surgery not for therapy or rehabilitation. An orhopedic surgeon knows more about surgery, chiropractors and physiotherapist know more about rehab and how to help lower back pain conservatively. That’s a simple fact. Now that you have the background.
Sitting is flexion just like downward dog. If flexion bothers you, Knee to Chest is also flexion. From my point of view I have a problem with this recommendation of knee to chest exercises and hamstring stretches as that also involves flexion. Also you get relief with standing which is extension. However I will say that I didn’t examine you and am only going by the information you have provided me.
In your case you are doing some exercises to relieve the problem and others that will aggravate. That’s just my opinion, however I have explained why I have the opinion that I do.
Hope that helps your disc herniation.
Hi Dr Ken,
I have found your site to be extremely informative and helpful. I have used many of the exercises listed here for the past 4 years as I have dealt with lower back pain worse than ever continuously almost Dailey. So I strectch and push through. Let me say that my back pain is actually more in the top of buttocks on each side of my spine. The majority of that time it was on the right more so.
My first bout of back pain was after a 4 wheel atv accident 20 years ago. I sprained my ankle, hurt my left knee and my right hip after falling backwards down a 30 foot incline. I was on crutches and PT for 12 weeks due to the back and hip pain, mind you I was only 13. After that no pain in back except when I over worked it playing sports or working until I was pregnant with my son at age 21. By my 8 month of pregnancy I had complete numbness of my right leg. Unable to lift it at all. I had to drag it up stairs and couldn’t leave lift my right foot to even put on pants, it just wouldn’t work. My Dr said it was sciatica and that the babies head was between my hips pushing on my spine and that after I delivered him I would be fine. True enough the dr was correct and it went away but I had mild lower back occasionally. I had a MVA at 22 and slammed into a cement wall. My back hurt but only after the paramedics laid me on the board for transport. I swear I felt a pop and my legs went numb. They did a bunch of X-rays and released me 8 hours later saying it was just muscle lock up from impact. Luckily I was okay and not seriously injured. During my second pregnancy 1 year later at 24 I dealt with LBP but no where near as bad as the first.
By age 28 I had LBP that would come and go. I called it my back going out. It usually lasted 4 to 5 days and then I would ok. During that time it hurt and burned and I used Otc meds to deal with it. I begain to exercise more, eat better, and stretch Dailey thinking that the healthier I got the better my back would be. This worked and my back would only go out occasionally. In 2011 I began seeing a dr for headaches who told me it was muscular and stress related due to my neck being straight and lacking curverture. I listened and continued to strectch. In 2011 I also took a job that required more sitting and computer use versus the jobs I had previously that required standing and bending. In 2013 I was rear ended in a minor MVA and it made my back flare up but I pushed through with tramadol and stretching. I was told by the same dr that my back issues where muscular. In sept 2014 I slipped on a wet floor and did a split. I hurt my left knee and ankle but I was fine. I told my dr that was sore but I could deal with it. In 2015 my back began to hurt a lot more and I would notice achy feelings in my legs. Dr said it was probably poor circulation and I should walk more and continue to strectch. I was also prescribed sleeping pills to help me sleep and gabapentin for nerve pain in my neck to help with headaches. During all this time I never missed work or went to the hospital for pain. The dr then prescribed narco 3 times a day and I stopped taking tramadol. I begin to notice that my leg/ foot would go numb if I sat on a hard surface and most especially during bowel movements. I also traveled a lot throughout 2015 for which required that I fly to meetings and would have to sit even more and the dr begin giving me shots in my back about every 3 months which did seem help with the flare ups and I noticed my back didn’t go out as much just dull pain I could handle. Dr said the numbness was due to sitting for long periods. Throughout 2015 I noticed I was stiffer in the mornings and my headaches became mirigrains lasting 2 days. I also noticed that my right toe hurt and I couldn’t apply pressure to it without sharp pain. My hips begin to hurt and my knees ached. I would strectch and I would stay active as I have an 11 and 13 year old who are very active in track, running 5 Ks and soccer. I work 6 days a week in a very demanding job that requires that I sit but I also get up and down out my chair 20 to 30 times a day and also outside client work which requires in and out my car several times a day. I took more vitamins and strectched more. I ate right and drink water. The last shot the dr gave me in oct 2015 burned very bad like lightening shooting across my hips and into my butt. He said that was inflammation and to continue taking NSAIDs daily. After that everything got worse pain was Dailey, legs were achy, hips were sore and stiffness was awful but I pushed through. The numbness started happening 3 to 4 times a week and was always from the knee down and now was both legs. Most especially while having bowel movements. In Feb 2016 I was walking down stadium steps and one step wiggled, I lost my balance and tried step with my left foot to regain it and then I opted to sit back to avoid a face first fall 15 feet down. I landed on my butt, bounced down to the next step. I was able to walk and had a huge bruise for 2 weeks. I iced it and pushed through. In March dr asked if I wanted an X-ray and I advised no as i knew I didn’t fracture anything because I could still walk. Since then the pain is also my left side too in my upper buttocks. Finally I convinced him that due to the numbness in my feet and legs during BM, and the fact my leg and foot was going numb at work also almost Dailey that I needed an MRI, during the Mri my right leg went numb this was in May 2016. I was unable to see my dr until 2 weeks ago at which the NP said they were referring me to a spine specialist and neurosurgeon. My mri results were disc dissection at l4 l5 with central disc protrusion and annular tear. Disc dissection at l5 s1 with paracentral disc herniation touching the left S1 nerve. They checked my knee reflexes at the dr office and said I had none and that I needed to be in to see the spine specialist and neurosurgeon within 2 weeks. My legs are achy and if I apply the brakes in my car at a red light my leg begins to shake. I am very concerned with the leg and feet numbness. The back pain is becoming unbearable and the strectching is only helping so I can get unstiffed and make it through work everyday. Resting makes my back hurt worse and walking is helpful. Can I still continue to use the strectching as long as they don’t hurt me worse and is the numbness permeate? I appreciate your response and your site very much.
Thank you.
Author
Thanks for your question Brandilynn. You don’t say what you do in the stretch. Maybe you are doing 2 stretches that are helpful and one that makes you worse but overall you feel better. I can’t tell you unless you tell me the specific stretch.
Hope that helsp your herniated disc.
Wow, you sound like me:) prayers for recovery
Author
Hope your disc herniation gets better as well April.
hi,i have l5s1 disk extrution and spinla stenosis-afte 6 week of physiotherapy and rest my back pain gone buy i still have a little pain somtimes in my left leg
-can i go back to gym with avoiding of squat and dead lift and bent over trains ??
-wich exercises i must do that push back disk ?
_any advice u may have
tnq
Author
Thanks for your question Babak. If the physiotherapist has already made you better than usually you stick with the exercises they gave you. They should also know the exercises that will continue to get you better going forward if a change is warranted.
Hope that helps your L5S1 disk extrusion.
tnq dr ken
do you hace any comment about discogel???
Author
Thanks for your question Babak. The research seems to indicate that it is helpful for disc herniations. I would do conservative therapy first though before doing any type of injections. First of all if you are injecting into the disc you have to damage the disc and create a hole. The disc does not repair itself unlike any other tissue in the body as there is no blood supply. Once the hole is created it remains. Also the studies are small and I am weary about who funded it. Also you don’t know if you will have a reaction to the substance. There can be allergic reactions to toxicity problems. It is certainly untested and one study does not mean it’s proven.
In summary always do conservative therapy first. Then injections that are proven then surgery.
Hope that helps your disc herniation.
In my mri report there are seggestive of mild posterior disc bulge at L4-S1 and L4-5 level…. What should i do …i feel pain in my right portion of lower back… I cannot walk and sleep well…. What i do… And suggest me the treatment plzz
Author
Thanks for your question Mayank. There are over 500 comments here. I suggest you read some. I don’t make recommendations unless you have given very detailed history of your symptoms.
Hope that you understand to help your possible disc herniation.
Hi Dr.Ken
Gratitude ? Thank u for helping people ….
Impressions of my MRI report
1) sacralized L5 vertebral body
2) L4-5 disc dessicatiob with posterocentral and left paracentral disc protrusion indenting thecal sac..No significant thecal sac or nerve root compression ..
I request you to kindly explain this and also its cause and effect and treatment for the same ….
Thank.u so much doc and wishing u abundant happiness and success….loads of prayers
Author
Thanks for your question Bhairavi.
1. Sacralized L5 means that instead of 5 lower back vertebrae one has fused to the pelvic bone so that you now have 4 lower back vertebrae. This causes the 4 remaining vertebrae to work harding usually leading to early degeneration of the disc above namely L45.
2. After some time the disc degeneration can manifest as a disc herniation.
Hope that helps your disc herniation.
Hi..this is sunil 39years old..I am having a polio in my left leg. Ten days before I had a severe back pain . After 2days I went to doctor and had a mri.the report says L4-5:diffuse disc bulge without any significant/foraminal stenosis….large leftparacentral disc extrusion at L5-S1 level causing significant central canal stenosis.causa equina nerve root compression and possible impigement of left S1 transferring nerve root…..doctor suggested for immediate surgery… now I am having a little pain in my back .my left leg ankle has become little bit weak and little bit numb and I can walk but my walk has altered please tell me should I have surgery
or not .if not give me other
suggestions…thank u
Author
Thanks for your question Sunil. In your case it looks as if surgery maybe an option. The fact that you didn’t already have surgery means it’s not an emergency but it looks urgent. You should get an examination by a person that can actually examine you.
Hope that helps your disc herniation.
Great article! I have been having the following problem for two weeks. First of all, I have priformis syndrome on both sides that I manage with massage and stretches. Piriformis is tender. on both sides but i managed to avoid sciatic pain by being careful about not externally rotating my hips and not tucking pelvis aq had been my habit for years. I ran 10k once a week with no problem as long as I paid attention to stride. MRI a few years ago showed slight disc degeneration and slight bulge L5S1, but it wasn’t pressing on the nerve and was due to left hip shifti g slightly backward and tendency to lean into the left leg, all of which i have tried to correct. I also have laxity at the pubic symphysis. I sensed that my pelvis was “off” bc of groin pain t certain moments but that only lasted a second. My right quad regularly felt slightly inflamed. I realized i was leaning into that leg at keeping knee bent to avoid sciaticic pain from left piriformis. Two weeks ago, i was running and felt numbness in right groun snd inner thigh. I immediately stopped running. I consulted a GP and later an osteo and am scheduled for tests. Seems like compression of the femoral nerve. The thing is the leg feels numb (a little) every time I walk. Feeling returns every time i sit or lie diwn. Would that i dicate the iliacus or psoas rather than a disk problem. The problem is – now the disk bulge on left side is causing slight sciatic pain. My auriculotherapist confirmed and i can tell she is right because the pain is exacerbated by forward flecion and sittibg up straight. Tried Mckenzie extension but seems to hurt the right side. My mris are not for a week and i was hoping to speed up healing but am at s loss. I do bird dogs which seem to help and also have q’ inversion table which seems to help. Sorry for presenting thiscomplicated issue to you. Happy 4th!
Sorry for all the typos on the last comment. I am typing from my phone. The other thing I forgot to mention is that the numbness changes in the left leg. Sometimes it is the ankle, but not the inner thigh. Is this strange. Thank you in advance.
Hello Dr.
I felt pain in my lower back a month ago and MRI report says ‘ small L4 disc herniation ‘
I am 22 and software engineer. Two bad habits are long sitting and driving. Dr advised me bed rest rest for a month. Now I am feeling pain free and have started walking. Sometimes when I take stairs, i feel a light pain and feeling at lower back. Should i avoid stairs ? And every time a disc patient feel this using stairs or it will get normal with time ?
If there is no pain , can I do exercises you mentioned in part 2 ?
And can I do gym/workout or not ?
And please guide can spine patients wear magnetic belt .
Thanks
Author
Thanks for your question Hussain. First if you go back to your old habits the problem will likely return.
1. You should try to go up the stairs with out bending forward which is what you are likely doing.
2. Yes do part 2 exercises.
3. You should avoid deadlifts and squats, bent over rows and rows.
4. I haven’t heard much about magnetic belts so I cannot advise you that.
Hope that helps your disc herniation.
Thank you so much for all your information and help given so kindky to everyone who asks. I’m not sure if you can help me but I am unable to lie down because that’s when the pain intensifies so much it has me screaming in agony. After nine nights of sitting in a chair to try and sleep but averaging only two to three hours in 24,I am really tired and would love to lie down and get some sleep. Do you have any idea of how I can cope with the pain so I can sleep?
Nine days ago after rising from a chair I felt pain in my lower back which within ten minutes became excruciating and radiated right across the right buttock and all the way down the outside of the right leg to the toes. The small toes and outer part of the lower leg became numb. I had v never had anything like that happen before though I do have a history of sudden onset back pain which usually clears with walking.
For the first two days i also had problems urinating but no numbness there. Even so, my GP thought it best to check for caudra equine syndrome and sent me straight to the hospital where i had a medical history taken and was thoroughly examined including a pin prick test and an internal to check bladder muscle tone. All was normal though the left side responded stronger than the right to the pinprick tests. The spinal surgeon thought it was a prolapsed disc at L4 L5 and I was sent for an MRI two days later to confirm this – but was still in such pain I was unable to lie still for more than a few minutes at a time so it had to be conducted in three parts. I was warned I might need a second MRI under sedation.There is a two week wait for results.
I am 71 and very overweight not helped by intermittent exercise because of extreme tiredness due to 20 years Sarcidosis .
The surgeon says I am not a candidate for corrective surgery and I do not like the idea of taking painkillers for the rest of my life so my plan is to consult an chiropractor once the MRI results are through
I am not currently taking any medication though I’ve tried stronger painkillers to see if they would help with the pain. They didn’t.. Ice packs sometimes help as can heat pads. Massage is too painful.
Hope I’ve presented a clear picture. Thank you in anticipation of any help you can offer me. I just want to be able to lie down ans sleep!
Author
Thanks for your question Phoebe. Try this to help you sleep. Put two pillow at your hip level and lie face down for about five minutes. After 5 minutes or whenever your back feels settled take one pillow out. Than after about another 5 minutes or whenever your back feels better take out the next pillow. At this point you should no pillows and should be lying face down. Stay there for 5 minutes or until comfortable. If at any point the pain gets too much put a pillow back under. The goal is to get to no pillows.
After that you should be fine sleeping in most positions. Don’t sleep in the fetal position.
Hope that helps your sleep due to pain from your disc herniation.
hi Sir
Thank you for your helping efforts for humanity.dr.ken ,I have acute slip disc on my lower back since 18 may2016.
I am under homeopathic doctor’s treatment from one month.I feel good but some times I have a little sweet pain on lower back and a pinching sensation on my buttock.
The doctor has asked me to avoid any yoga or exercises when he is treating .
I am very worried about this injury I know well that slip disc is a curse.
will I get 100 percent recovery in any condition ?I am 28 years old .
should I walk for a physio…
plz suggest ,what should I do?
Dr. havent ask for MRI.
WITH REGARDS
Author
Thanks for your question Krish. I have never heard that a slipped disc is a curse. I have a slipped disc so I must be cursed too and I didn’t even know it. Krish, that’s pretty dramatic. Your expectations of your curse is also very high. 100%. Lower back pain by most causes is usually comes back over and over again. Usually because we keep aggravating the problem without even knowing it. For most people it’s bad posture, sitting and bending forward to wash their face, putting on your socks, shoes. Anything that is bent forward. For the most part people aggravate their own back.
So 100% is no very likely. Most people don’t have perfect posture and consistently aggravate their backs and don’t do the exercises. However if you have better posture, don’t aggravate your lower back and do the right exercises you can manage your lower back. It may even go away for a year, 5 years or 20 years and likely come back in a different way. So can the pain go away 100% absolutely but are you 100% cured no. It really depends on what you mean by 100% recovery.
https://www.bodiempowerment.com/herniated-disc-part-2-the-best-exercises-for-your-herniated-disc/
Here are the exercises you can do. As with any exercises you can get worse so you need to have these exercises supervised by a chiropractor or physiotherapist that knows these exercises. Hope you go to the best chiro or physio in your town. You know you are getting worse if the pain starts going further down from down into the thigh or leg. If that happens you need to stop.
Hope that helps your disc herniation.
Dear Dr Nakamura, are these exercises also for a bulging disc in the neck? I neck refers pain in between my shoulders & down my right arm. I’m having a bad bout at the moment. We had lots of sports at my daughter’s school of late, so sitting on funny chairs & benches for hours. Regards. Anita Hapelt
Author
Thanks for your question Anita. No here is the link for a bulging disk in the neck or cervical disc herniation. https://www.bodiempowerment.com/cervical-disc-herniation-best-exercises-help-sore-neck/
You really should have it looked by a professional as just doing exercises may make you worse.
Hope that helps your cervical disc herniation.
hi Dr Ken I have L4 L5 disc herniation protrusion shown on MRI I have pain in butlock when trying to walk or sitting for a long time when I try to stand up straight the pain in the buttlock gets realy bad to the point that I rather bend a bit I have tingling and numbness in the right foot mostly the small toas . I have been resting in bed for the past 5 weeks am I going to get better ?
thax a lot
best regards Fari
Author
Thanks for your question Fariborze. You really have to see a professional in your case that being the best chiropractor or physiotherapist in your area. Your disc is out quite a bit. Most of them can straighten you out and decrease your pain. Remember though it really is how good they are not the name of the profession that is important.
Hope that helps your disc herniation.
Hello Dr. Ken,
I have disc prolapse in 2006. Symptoms were like radiating pain in right leg. Little numbness, severe sciatica nerve pain. MRI done at that time says disc degeneration with broad base posterior prolapse at L4L5 L5S1 levels indenting the theca and narrowing the neural foramina bilaterally. After taking conservatory measures I was cured to 90%. But suddenly the same pain started in 2016. Yes I have not been doing exercises for spine last 3 years religiously. Now I curse myself. Consulted with doc. Suggested me to take rest for 4 weeks. Now symptoms are like radiating pain in left leg. Mild calf pain. Sciatic nerve pain. I was tied to bed for one week. But now I can walk for 10 20 minutes with mild pain. Very painful sciatica nerve pain has somehow subsidised. So I want to exercise please help me. I am a office goer, I have to sit at least for 6 hrs. No problem in bowels and bladder. No foot drop. Mild numbness in foot fingers but not always. Do you think I am a candidate for surgery? If no then please help me with some exercises and when to start doing. After 4weeks or to wait till pain subsides.
Author
Thanks for your question Arjun. Sounds like you have been reading the comments. Try these exercises. https://www.bodiempowerment.com/herniated-disc-part-2-the-best-exercises-for-your-herniated-disc/
These exercises must be supervised by a health practitioner as they can make you worse. Hope that helps your disc herniation.
Great article.
Sir , kindly give your email where I can contact you about my problem
Author
Hussain, I don’t give out my email. If you want help you can ask on this forum, if you don’t want to, I cannot help you.
Dear Dr,
I felt pain in my back few months ago. I ignored it and after some rest I felt much better, but few days back I felt pain at my lower back leading to left leg so I went for MRI. “A small L45 disc herniation” was written on report by DR and he advised me one week complete bed rest. Now I am feeling much better. I am only 22 yrs old and I took no medicine or pain killers. I studied exercises and your blogs and research which helped me a lot.
I am a software engineer and I think usually prolonged sitting and driving is the main problem in my case as I travel a lot.
Need your advise ..
– What measures should I take while driving?
– To avoid future risk and pain, what should be my posture for sitting on chair?
– what are the basic wrong exercises that I should avoid in Gym.
Will be waiting for your answer.
Thanks a lot Dr for your articles because I have learnt a lot from that .
Dear Dr. Ken, pls help.
I feel i am at the right place right time.
I am 44 years, female.
On 20th may 2016 , as usual i did some yoga stretching touching toe etc. Suddenly sever back sprain hits me and i was unable to even move. Movement was completely arrested. Not take even a step. I was rushed to hospital and and mri was done, and the report says
1. Lumbar spondilosis
2. Mild central and left central disc protrusion noted at l4 l5 level indenting thecal sac with no signifacant narrowing of thecal sac itrapedicular neutal foramina or lateral recesses.
3. Central , left central and sabatical disc extrusion with inferior migration.( up to mid s1 body level) noted at L5 S1 level indenting and narro ing thecal sac and left lateral recess compressing teaversing left s1 nerve root.
Doctor has advised to be on traction for 2 weeks. (6 kg.) And doing physiotherapy currenly.
Kinldy advice . Will this treatment suffice? What changes i need to make on life style
159 cm height mostly on sitting job, weighs 63kg.
Else i am a regular exercising person
Author
Thanks for your question Anjali. Yes it’s true as I have said in many of articles, yoga causes many people back problems.
Traction does help some people, I would give it a try along with the physiotherapy to see how it all goes.
Hope that helps your disc extrusion.
Thank you very much Doctor for the reply. Now its over two months since the first occurance. Now my problem is , i am having slight irritated pain on my left leg always. Kindly advice on what are the next steps to be taken .
Will doing the prone McKenzie help?
Author
Thanks for your question Anjali. Are you better? slightly better? A lot better?
I am a 53 yo carpenter and have recently(4weeks ago) developed a 1/2″x3/4″ L5/S1 disc prolapse with compression to the right sciatic nerve. Surgery has been advised but I prefer to to go the non evasive path. I have occasional tingling on the right side of my right foot and leg and can walk around comfortably for short periods of time until right buttock pain forces me to lie down and the pain disappears shortly after. My main issue is that I can’t sit down or drive for more than a couple of minutes without the pain in my right butt becoming intolerable, my physio suspects that it’s caused because the nerve movement is restricted at the bulge so the sciatic nerve is trying to stretch at the pyriformis muscle(there is local swelling and tenderness there) this is highly restricting. I am doing a major core exercising routine daily including the excercises that you recommend without pain and there is improvement in all areas except the ability to sit. Do you have any suggestions?
Author
Thanks for your question Paul. Why don’t you try an ART or active release therapist for your muscles. I often find that releasing the muscles helps tremendously even though you are not treating the cause when you do this.
Hope that helps your sciatica.
Hiiiiii sir, my self sachin n thawal age 23 from pune district Maharashtra sir my problem of back pain and L4 L5 pivd n left foot droop
Author
Thanks for your comment Sachin. You need to find a professional as exercises alone won’t help you.
Hope that helps your foot drop.
PLEASE PLEASE give me some advice. I’m a 43 year old healthy female and my history with a my L5/S1 are as follows: March 2015 I woke up and had lower back pain that in a few days moved down my left side. The pain never went away, it way day and night. I had a MRI which showed L4 & L5 are degenerated and L5/S1 is herniated so, a week later the doctor performed a Laminotomy and Microdiscectomy. I felt immediate relieve when I woke up from surgery. I couldn’t believe I was pain free. I recovered 6 weeks at home with a lot of laying. During these 6 weeks I took no pain meds because I didn’t need it. I didn’t have leg or back pain but I did have pains from simply laying so much. Everything was great for about 16 weeks and one day at work I was in an twisted awkward position pulling something and I felt a pain in my back. My back was sore for a few days and then the leg pain started again….the exact same pain I had before. I had another MRI that showed I herniated the same disc but the herniation was bigger than the first one. So I had the same surgery with the same results…pain free once again. However, this time I didn’t lay so much. I was careful with my activities and conscious of my movements, but tried to be more active this time after surgery. Again everything was great for 16 weeks and one day my left side started having extreme pain. I didn’t think it was possible to feel more pain but this pain was was worse. My doctor admitted me to the hospital from the extreme pain I was in and he wanted me to have an MRI immediately to see what was causing the pain. The MRI showed a very small herniation for the 3rd time on the same disc. Needless to say not only was I in pain again, but was devastated to get this news for the 3rd time. While I was in the hospital the doctor started me on 1200mg Neurontin/Gabapentin, I received steroids intravenously and had an epidural. The doctor recommended a fusion and rods. So I’ve been out of the hospital for a week and half and I’m not in as much pain as I was before my hospital stay however, I’m not pain free. I didn’t expect to be pain free either. I feel the epidural combined with the Neurontin may have lessened the pain but I don’t like the side effects from the Neurontin. I think I’m still young a young 43 and I don’t want to have the surgery! I’ve been researching any alternatives (exercises, acupuncture, acupressure, TENS unit, massages, and natural medication). For the past few days I’ve been walking and doing a few prone exercises and I feel a little less pain. I don’t have the shooting electrical pain without my movements causing it. I would have this pain every few minutes before with and without movement. I don’t want to believe or accept that a fusion and rods are my only options in spite of this recommendation. My research for an alternate route has led me to you and sending this message. It my cry for help! Please give me your advice based on my history. THANK YOU so much.
Author
Thanks for your question Stella. I question your surgeon. Was needed in the first place? Here are the criteria for surgery.
1. Bowel or bladder not functioning properly usually bladder retention (cannot or hard time starting to urinate)
2. Saddle anesthesia which is numbness, tingling around the buttocks, groin and inner thighs (basically where a saddle would touch)
3. Deteriorating neurological symptoms like a foot drop or muscle wasting that was getting worse.
If you didn’t have any these above and you didn’t do conservative therapy before surgery then proper protocol was not followed. It doesn’t sound like any of the protocols were followed and sounds very suspicious to me but you know the details of your case.
I have exercises in part 2 here https://www.bodiempowerment.com/herniated-disc-part-2-the-best-exercises-for-your-herniated-disc/
However I don’t recommend them as you will better off with the best chiropractor in your area or the best physiotherapist.
Hope that helps your disc herniation.